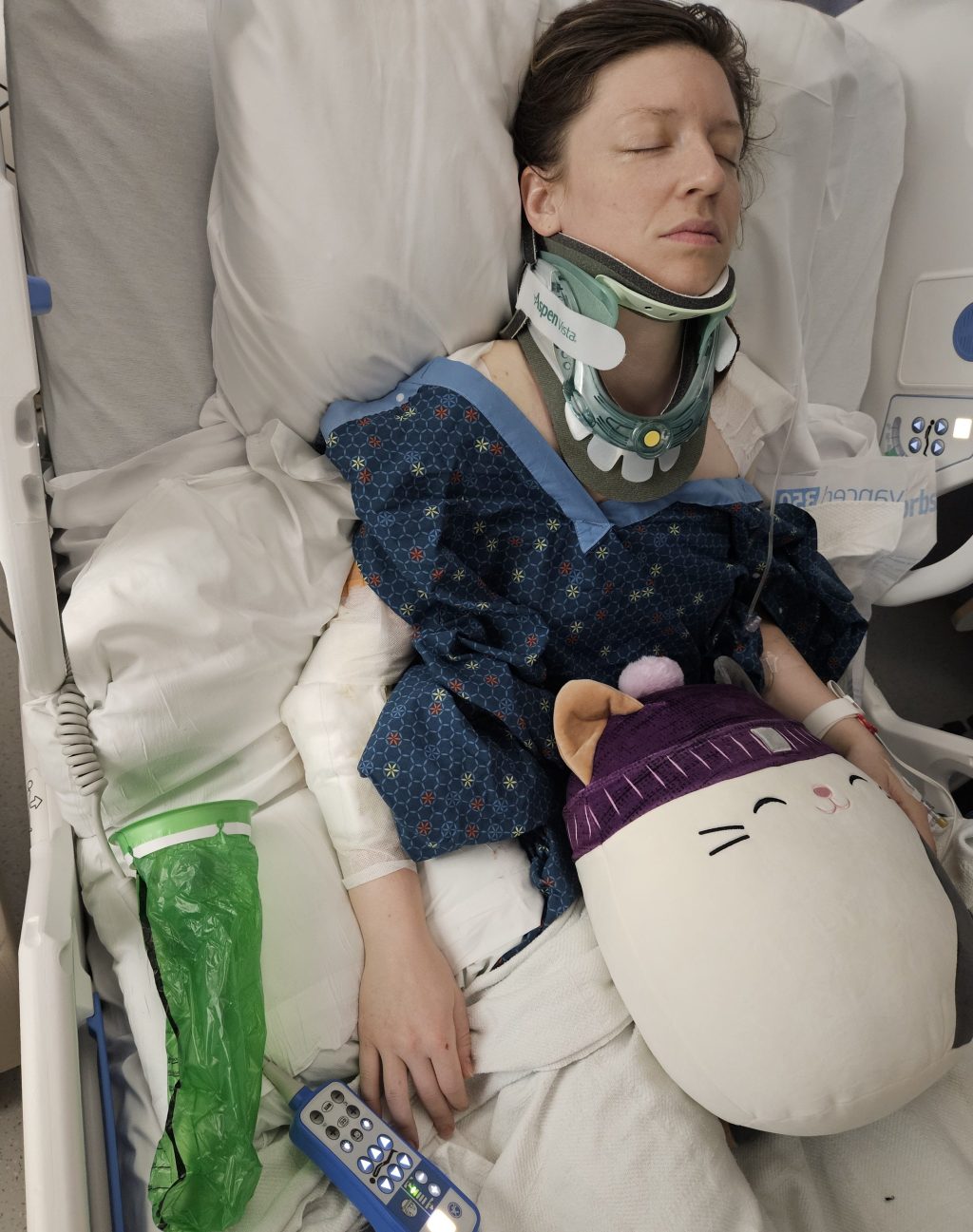
My 2025 Season Takeout.
(content warning)
Part 1: The Crash (April 2025)
I became conscious already having made impact on the far right side of my head. The overwhelming weight of my body continued to grind forward with the sound of plastic scraping against the pavement above my right ear. I continued to drag across the ground long enough to become aware that I was crashing followed by thoughts of how I would prefer to stop crashing. I was decelerating from our 30.3mph paceline, watching in slow motion as two other cyclists dodge below my legs. The next thing to follow was the heavy impact of the cyclist behind me who ramped off of my torso into the far lane of traffic. My body was sent forward like a ragdoll, flipping several times before somehow landing in a seated position just to the right of white line off of the main road. My bike was nowhere to be seen. I continued to watch the carnage unfold as others were crashing into the grass on my right and into the road on my left. I heard the yells of my friends and others who quickly took action to stop traffic and seek help. I then saw my friend Sam not moving on the ground about twenty feet ahead of me. I recentered my focus to myself realizing that I could be very injured. I sat breathing fast, internally scanning by body head to toe. As a physician assistant, I was trapped somewhere between patient and provider. I felt dazed and heavy. I recall thinking “I’m alive”, followed by “I think I’m okay”. In taking my next breath, I felt an unsettling shift along my rib cage and I wasn’t able to move my right shoulder. I then knew that I wasn’t okay. I attempted to call my husband, Kevin, but did not have any cell reception. I overheard someone say 911 was contacted. I was on autopilot asking for someone to call my husband, repeating his cell phone number over and over in a manner too fast for anyone to understand. A fellow rider graciously took my phone for his number and was able to get a hold of him. Kevin later admitted in the most realistic sense that receiving this call wasn’t a matter of “if” but “when and how bad”.
The next group of riders showed up on the scene only a minute or two behind our group. I was able to find some comfort in seeing fellow cyclists, Kris, who happens to be a physician, appear in front of me. I was so thankful for her presence and her willingness to sit by my side until emergency services arrived. She assured me that our friend Sam, still lying motionless, was alright and continued to convince me that I would be as well. It felt like eternity for the ambulance to arrive as I did my best to control my breathing and block the worst case scenarios from entering my head. I wasn’t in pain per say but my body felt very unwell, almost on a subconscious level. Kris confirmed to me that my clavicle was toast. She gently cut the right shoulder strap off of my clothes to alleviate the tension on the fracture. I reached up with my left hand to assess the damage. I felt the slightest bit of skin tented up and immediately retracted. It was more than I could handle right now. Once medics arrived, I was first to be loaded into the ambulance. I felt a sense of relief that I was one step closer to the hospital.



Part 2: The Emergency Department
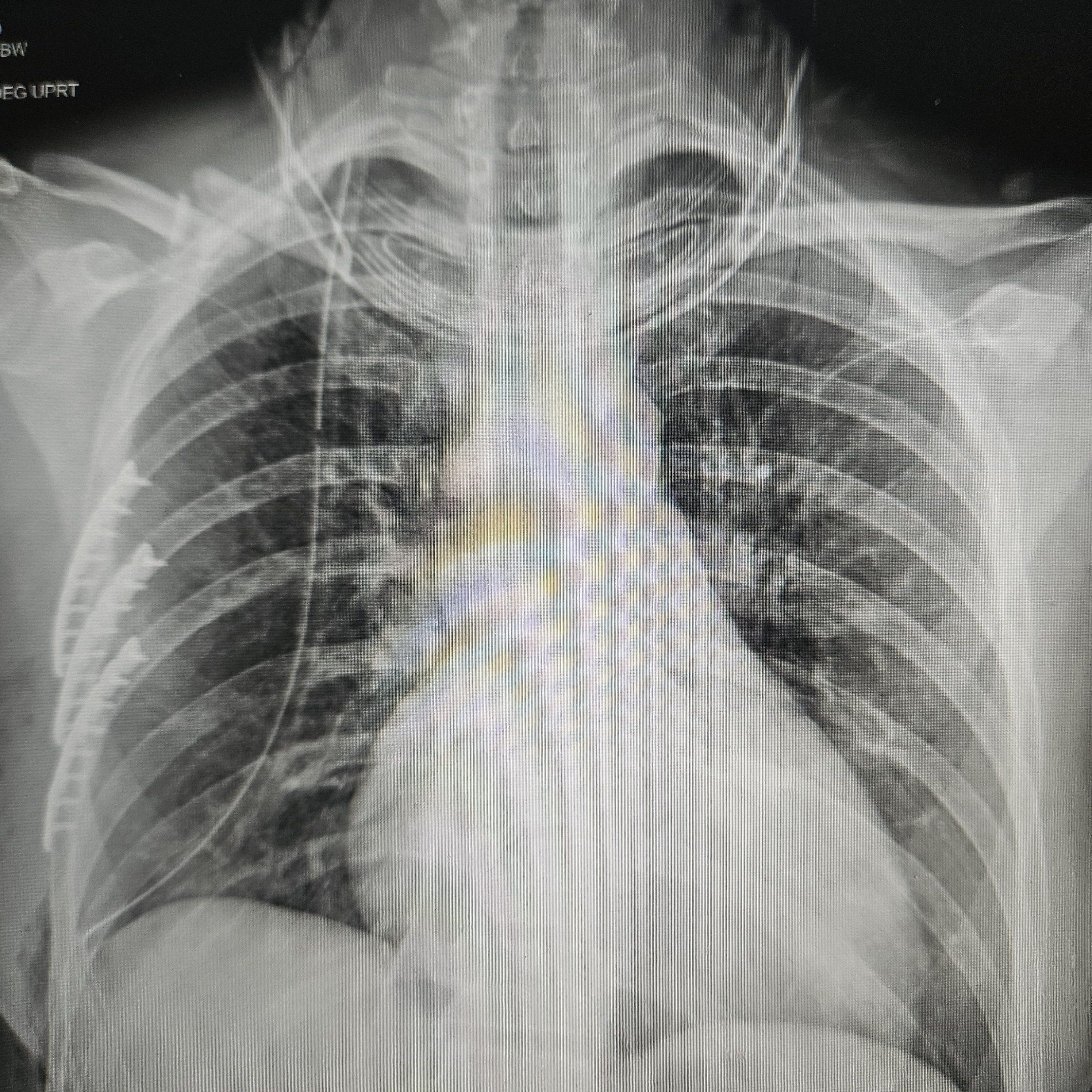
My husband was walking up to the trauma bay as I was being unloaded from the ambulance. I was happy to see him as I’m sure he was happy to see me in a stable condition. I may have been a little too happy after the pain medication I received enroute, joking and bantering with the medics. I was wheeled into the Emergency Department where the entire trauma bay was lined with hospital staff dressed in their yellow gowns and gloves also unaware of the extent of my injuries. They transferred me onto the hospital bed and immediately placed a rigid neck brace on in exchange for the softer version I had in transit. I knew my bike clothes were a goner. They graciously asked if there was an easy way to remove my heart rate monitor so they didn’t have to cut it off. I appreciated that. All the staff were then working in sync to complete their head to toe assessment. There was so much happening all at once and yet all I was doing was laying there: One provider was looking in my right ear while another was performing an ultrasound on my abdomen, and another assessing my leg wounds. I hear someone say “x-ray” followed by the beep of the machine shooting. Someone else was asking me questions about what happened and what I was feeling. There was a short argument over where my helmet was as the providers wanted to map out the damaged sites. Meanwhile exam findings were being yelled out to document. I hear someone say “right pneumothorax” (air trapped around the lung space). I immediately became nauseated and frantically asked if I would need a chest tube. Thankfully one of the workers noticed my distress and assured me that the pneumothorax was small and I wouldn’t need a chest tube for now (I later would).
As soon as they finished their initial assessment I was taken for a full body CT scan, then another CT, and then an MRI of my head and neck. It should have been a bigger red flag to me as to why they were looking at my neck so closely. But I was just at the mercy of the gurney. What ended up being hours felt like minutes. I gathered as much information as my brain would let me. Once all the scans were complete, the extent of my injuries were confirmed to be a broken right clavicle, four broken ribs (ribs #4-7), lung contusions, small hemopneumothorax (blood and air trapped around the lung), large right gluteal hematoma, and scattered road rash down the right side of my body. I asked if I could have the neck collar off to which the response was Neurosurgery needed to see me. At that point I put the pieces together that something was wrong with my neck. The good news was Neurosurgery came quickly and confirmed that I didn’t break my neck. The bad news was that I herniated a disc which was pressing on my spinal cord. That was the last I saw and heard from Neurosurgery during my hospitalization. I wasn’t told of the concussion diagnosis until later. I initially thought I lucked out by not getting one but it was so obvious that I had a concussion that it just wasn’t said out loud. My concussion symptoms became much more pronounced in the following weeks.
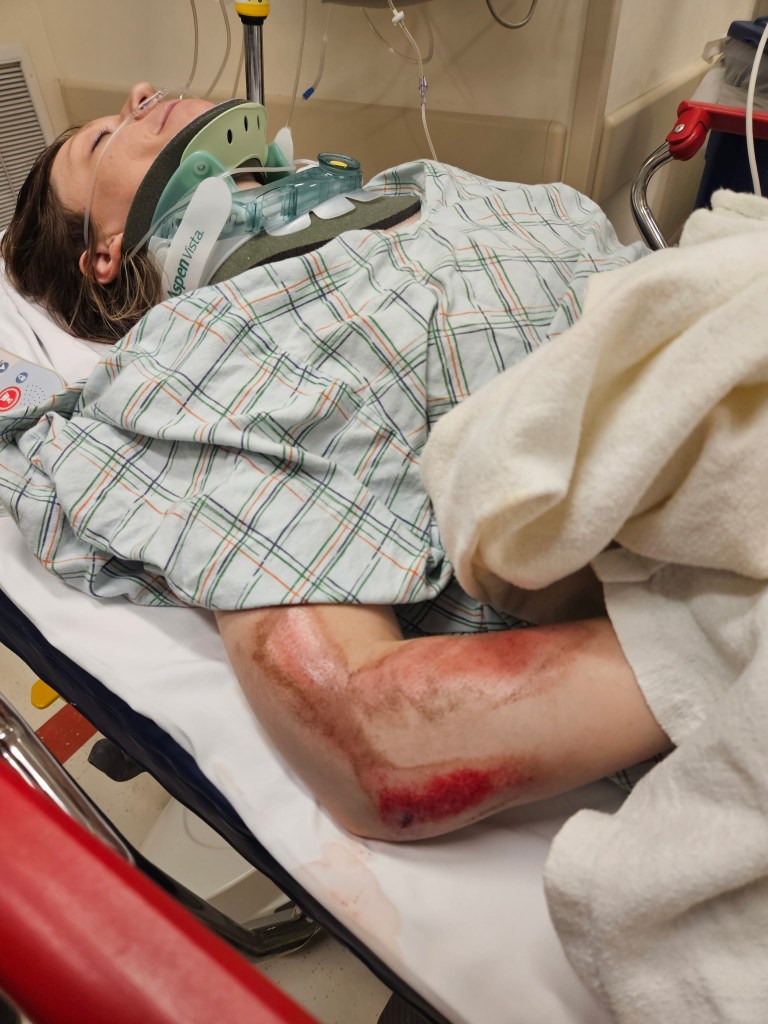
Eventually the chaos of my evaluation died down and the focus was drawn towards the next trauma patient. Sam was two trauma bays over. I could pick up bits and pieces of what was happening to him. We learned that he shattered one of the bones in his ankle. At one point, I recall Kevin making a very concerned face watching the ED staff attempt to manually reposition his ankle. Sam’s wife, Becky, showed up at some point. Kevin and Becky essentially merged into one support system between Sam and I. My mother later arrived to become a third party in this support structure.
I was taken out of the trauma bay and wheeled to a small curtained room awaiting an inpatient bed. I had no concept of time. I’m not sure if I slept. It was dark. Kevin was there or he wasn’t. The patient next to me was coughing a lot. I remember thinking I hope I don’t get sick being next door to this patient. He was later discharged. My first visitor appeared early in the morning. Around my curtain appeared Brian, an anesthesiologist I knew from work and also a cycling friend. Word of my crash travelled fast. Turns out Brian was way less excited to see me as I was to see him. This wasn’t a social visit, I was his patient. That’s when I learned I would need surgery to repair my broken clavicle. Next to appear was my good friend Lindsay who also happened to be a CRNA at the hospital. She was off that day but graciously dedicated her time to help coordinate basically my entire hospital stay (forever grateful to have her as a friend). I was surprised by the next team who appeared at my bedside, Thoracic Surgery. They recommended plating some of my ribs. My drugged and concussed mind was shocked at this recommendation but they felt surgery was necessary given my arm instability and the displacement of the ribs. Honestly, I ended up moving forward with the surgery because the idea of being under anesthesia was lovely compared to the discomfort I was in awake. I was taken to the OR that afternoon.
Part 3: The Hospital
I woke up in the PACU (post anesthesia care unit), coming out of anesthesia with one of the most vivid dreams I’ve ever had. The dream was reminiscent of Ms. Frizzle in The Magic School Bus where she takes her students on a ride through the human body except it was me and I was inside of my own leg. I woke up so excited to see several of my friends/coworkers at my bedside. I instantly felt the stability back in my arm and chest wall. But my chest felt a little tight and taking a deep breath was nearly impossible. That’s when I realized I woke up with a chest tube. I was informed later on that there was a puncture into my lung space from the ribs so in addition to plating three ribs, they placed a camera into my lung space to assess the damage and clean it up. The chest tube was to make sure any residual air and blood could make its way out. I wasn’t wrong in my fear of having a chest tube. That was hands down the worst, most painful part of my injury. Luckily it remained in for less than 24 hours. The relief was immediate on removal.
After my first surgery, I was transferred to an inpatient bed and placed in a joint room with an older lady. It was a little disappointing to be in a double room, but honestly, I was probably the bad roommate as I had so many visitors throughout the day. I was beyond excited every time one of my friends stopped by to check in. It was equally an uplifting energy boost as much as a distraction from the situation. I felt incredibly supported by my community: my husband, my friends, my work family, my bike family, and my mother who drove 10 hours to be by my side. The volume of love and support was something I had never experienced before. It wasn’t hard to make the best of a bad situation.

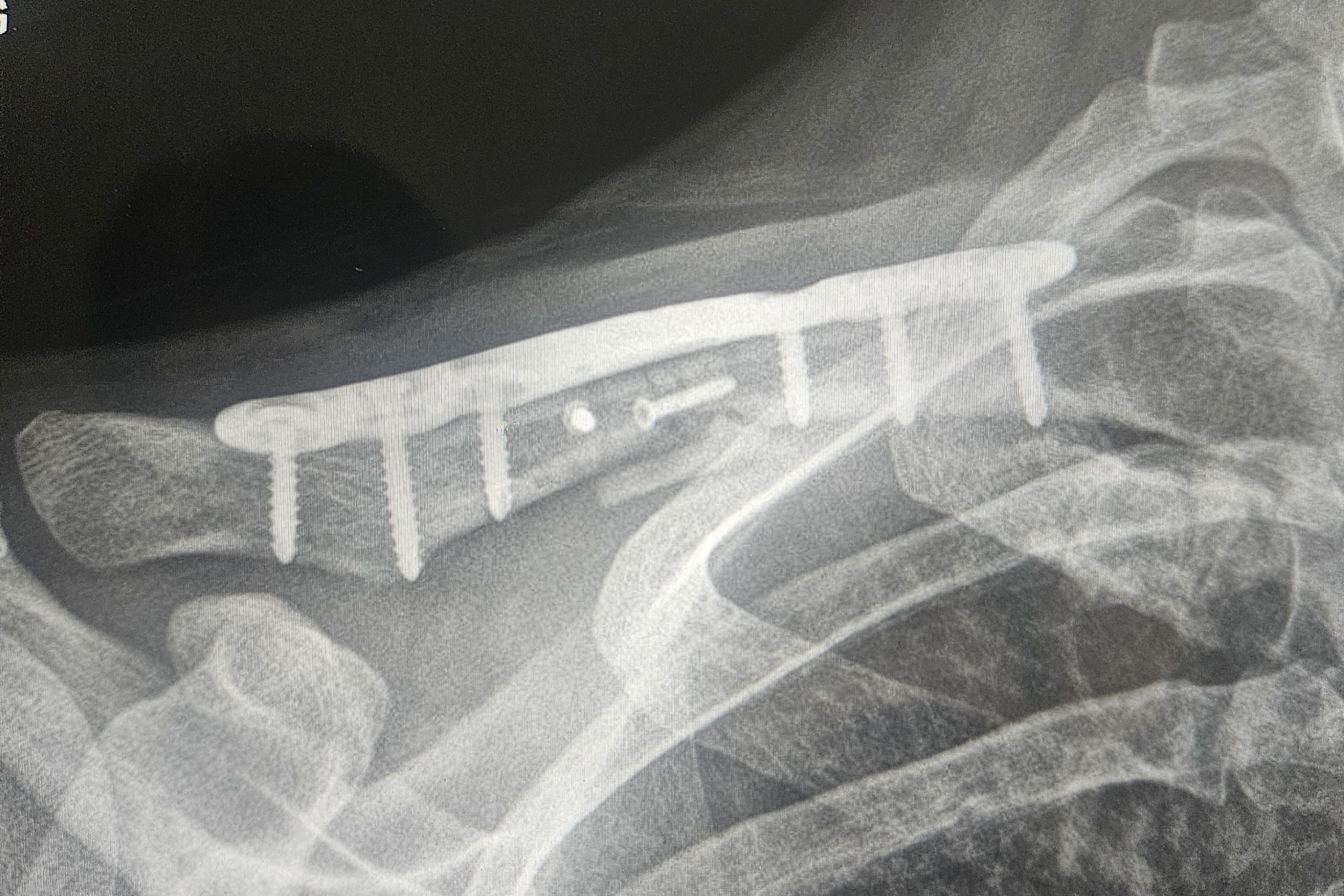
Day three of my hospital stay was my clavicle repair surgery. My top tier anesthesia team, Brian and Lindsay, were ready to put me under for round two. I was taken to the OR where I’m pretty sure I fell asleep before they even placed me on the OR table. I don’t recall very much beyond that point. After surgery, I was taken back to the same room I came from. The rest of the day was pretty blurry after my second round of anesthesia. My trauma buddy Sam was admitted to the same unit awaiting surgery on his ankle. He was wheelchaired to my room that evening to visit. I was so happy to see him doing well but was too drowsy to stay awake for long. He did explain that he wasn’t moving at the scene of the accident to avoid the immense pain from his ankle fracture. He had his ankle operated on the day after I was discharged. Sam and I continue to send “happy crash-iversary” texts.
By the next morning I was out of bed for the first time since the accident. My clarity was coming back. It felt like such an achievement to brush my own teeth. Lindsay had thankfully braided my hair so I didn’t have to worry about it. Navigating the neck brace and my right arm sling was challenging but OT reassured me I would come up with creative solutions. I was up for discharge on my fourth day in the hospital pending I could walk up one flight of stairs with PT. I passed with flying colors. I was discharged shortly after.
Part 4: The Recovery
I spent the next week mostly on the couch running out of shows to watch on Netflix. If I wasn’t on the couch I was in bed with the head of the bed upright because I couldn’t lie flat. Kevin was forced to play nurse as I could only do 10% of tasks. I couldn’t lift my right arm at this point but my hand was functional. I had little core strength. Showering felt like a marathon. A shower chair and a shower head with a hose were a must. I was in constant discomfort, not pain per say, just very uncomfortable. Wound care seemed to be an endless task. Despite the deep (painful) washout in the ED, I continued to remove bits of dirt from my wounds for several days. It took over a month for the wounds to stop weeping.
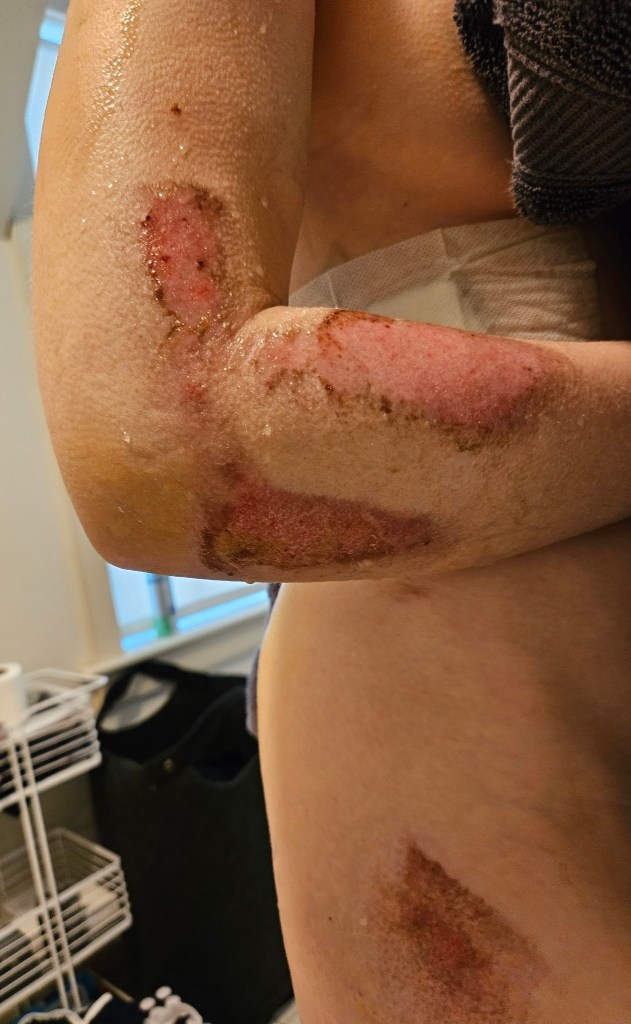
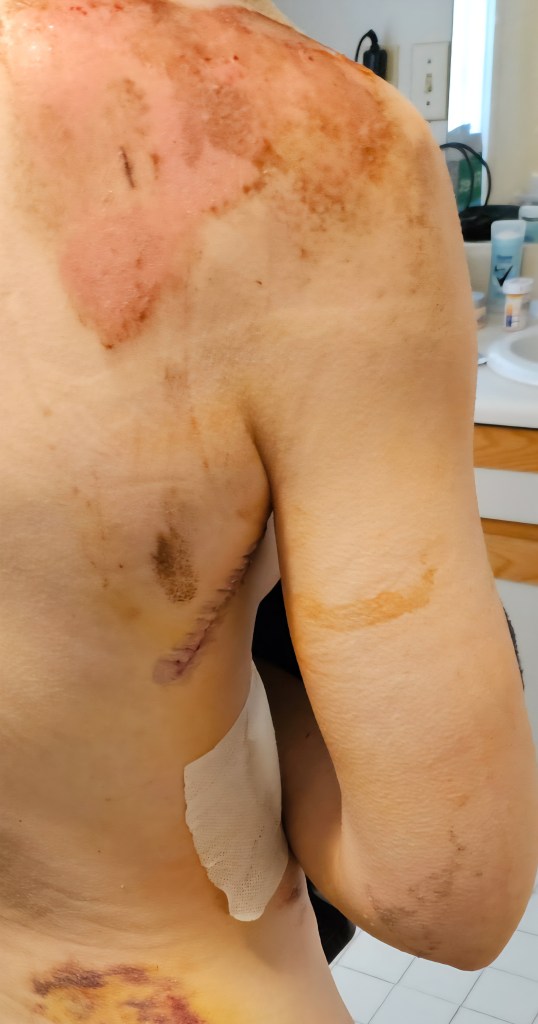
By week two I was able to tolerate going outside for short walks. I could lift my arm to 90 degrees at this point. I figured out creative ways to get my arm in the sling by myself as well as my neck brace. Doing my hair was impossible. Kevin tried his best to help but I ended up cutting my hair off instead. I started concussion therapy OT where I learned to identify my concussion symptoms and address them. I struggled with headaches and nausea triggered by stress/activity, lights, and sounds. Focusing on a present task was challenging. There was one instance where I walked into a store forgetting why I went in there. I couldn’t remember responses I had just told people like my phone number or my coffee order at the cafe. For a while I questioned everything I said. Not to mention the ongoing emotional swings. It was later on discovered that my eye convergence (inward movement of the eyes as objects come closer) was also malfunctioning. This made reading quite challenging, hence the lack of writing over the last year.
My endurance started to progress by week three. I took longer walks each day and eventually upgraded to short uphill hikes. My neck brace was removed after finally seeing Neurosurgery in clinic. Repeat x-rays showed my neck remained stable and my herniated disc never caused any symptoms so no further intervention was needed. By one month I was cleared to lift up to 10 pounds and use my sling as needed. I was allowed back on the bike trainer as long as I didn’t bear weight on it. At this point, I could lift my arm to 120 degrees. I went back to work on light duty one month out.


After two months I was cleared to bike outside with caution. I quickly learned how fragile my cycling capabilities were. I had spent the previous two years obsessed with cycling, training 5-6 days per week, giving up my weekends for endurance rides, and really prioritizing my racing goals over everything else. So much of what I worked so hard for was lost in seconds. It was a harsh realization. I wasn’t sure I even wanted to build it back at this point. But at the end of the day I still loved cycling. Three months in I went back to racing and competed in a Novice Class XC MTB race. I ended up second place. I wasn’t able to do more than about 90 minutes of mod-intense exercise without symptoms so my attempts at endurance events mostly ended in DNF or casual riding.
Five months of PT left me at about 95% recovered in terms of strength. My right shoulder soreness stuck around for a while as did the occasional zap of a nerve that was a casualty of the accident. I experience popping, “gristly” sensations in the muscles of my right rib cage/scapula. My incisions are well healed only leaving behind reddish hued scars. The silhouette of the titanium plate supporting my clavicle is visible since the swelling resolved but it isn’t too disfiguring. It took until mid-November (7 months) for my concussion symptoms to resolve. At that time, the riding season had pretty much come to an end.
Many people have asked me if I am afraid to be back on my bike or if I experience any PTSD. The honest answer is no but I never recovered the memory of the accident. I only things I remember are talking to the rider next to me and waking up already on the ground mid-crash. I’ve long accepted the risks associated with cycling. I would rather not go through this again, but the happiness and freedom I get out of cycling is worth the risk. I am SO grateful to be able to still ride and SO grateful to have experienced the mass support from my friends and family. I’m not sure where cycling will take me in the future, but it is still a large part of my life. Stay tuned for the next chapter!